Thirteen new patients were diagnosed with the coronavirus yesterday.
The latest cases included 12 more in England and the first patient in Scotland, meaning the virus has now reached all four parts of the UK. A health worker at an NHS cancer centre in Middlesex is also among the new cases. Another is a staff member at Wimbledon College in south-west London, which has closed for deep cleaning.
Three of the new cases in England were linked to a man from Surrey, who was the first patient to not have been abroad recently and was instead infected within the UK. This indicates that the virus has been under the radar within the UK, possibly for a matter of weeks.
Boris Johnson has warned today that the spread of coronavirus in the UK “looks likely” to become more significant in the coming days, after chairing an emergency Cobra meeting to discuss the government’s response to the outbreak, earlier. Health secretary Matt Hancock has warned it is now “inevitable” the deadly virus would “become endemic” in the UK.
Meanwhile, the global death toll from the disease has passed 3,000, with more than 80,000 cases worldwide. Several countries in Europe, the Middle East and the Americas have banned large gatherings and imposed stricter travel restrictions in an attempt to limit infections.
The first death from coronavirus (COVID-19) in the US was an eyeopener. Apparently, no-one is sure if it happened to a man or a woman. Donald Trump says a woman died who was “at risk anyway”. Other sources say it was a man. It shows the profound lack of sympathy, and a fundamental lack of concern and respect for people who have a medical condition and vulnerability to infection in neoliberal economies. Many people in the UK have known for some time that the UK government regards disabled and ill people as a ‘disposable’ reserve army of labor.
This virus has thrown the political indifference to ill, disabled and ‘economically inactive’ citizens into sharp relief.
The indifference is embedded within public attitudes in our society, too. I’ve seen many other people comment that ‘most people only get mild symptoms’ and ‘it’s not worth worrying about’. It’s just ‘scaremongering’ and ‘panic’ over nothing.
It isn’t, unless you happen to have a co-morbid condition. And those with only ‘mild’ symptoms unfortunately pass the virus to people who are ‘at risk’. Those who are lucky enough to be unconcerned about the virus should at least care about those who have reason to be very worried.
The government have so far refused to consider closing schools, because children seem to be at low risk of getting very ill with COVID-19 infection. However, they do get the infection and they pass it on to others – teachers, parents and grandparents. This means the virus won’t be effectively contained once it becomes transmitted within communities – and it will. In fact it has already happened. One man in Surrey has become ill, and has not travelled. No-one knows how he got the virus.
In China, it became apparent that many people had been infected before it came to the attention of the health authorities. It had already spread widely within communities. Because this is a virus that frequently causes symptoms very similar to mild flu or a common cold in healthy, young people, it’s very easily transmitted from person to person. This means it can easily go under the radar for a while. Italian scientists believe the virus was circulating there unnoticed for weeks, too. I should add that as yet, we don’t know if there are any longer term health consequences of infection for everyone, including for those who had mild illness initially.
There are also concerns about the impact of the virus on the economy. We have a work culture that encourages people to turn up to work with colds and other conditions, which is then shared around the workforce. It’s a culture that doesn’t facilitate consideration that some people are more vulnerable to serious complications from viral infections. The government are currently considering “the balance between public safety and economic and social impacts”, weighing it against the possible benefit of closing schools, stopping public transport, and activities involving large gatherings of people.
For the government so far, it’s business as usual.
However, the World Health Organisation (WHO) are now advising elderly people and those with chronic health conditions to ‘avoid crowded areas’ to reduce their risk.
So who is at risk of serious complications from the coronavirus?
How many people in the UK and US have asthma? All of those people are ‘at increased risk’ of serious illness and mortality.
How many people have diabetes, autoimmune illnesses, lung disease, heart disease or other underlying health conditions? Those people are all at risk.
How many are people taking immune suppressants, steroids or chemotherapy for illnesses or cancer? Those people are at risk.
How many people are clinically obese? Those people are at risk, too.
How many people are over 60? Those people are at risk.
How many people need an annual ‘flu shot? Those people are at risk.
That’s a lot of people.
And among those are people in your own families, and among your friends and neighbours.
The virus kills susceptible people because it causes pneumonia, respiratory distress and often disrupts the immune system, causing a ‘cytokine storm’ and severe sepsis. It also seems to cause a long term autoimmune-type condition in some people after they have recovered from the initial infection, even in people who have had initially mild symptoms. There is evidence that this coronavirus also infects and damages other organs, as well as the lungs.
For those who think covid is ‘just the ‘flu’, in 2017 I caught ‘just the ‘flu’. Within four days I developed advanced pneumonia, sepsis and almost died. I was so unwell with the ‘flu that I hadn’t recognised how seriously ill I had become, until I tried to get out of bed for a glass of water. By the time the paramedics arrived, I was already in septic shock. The prognosis following tests and an X ray were not good.
I survived and recovered only because I got a prompt diagnosis and prompt treatment, which included intensive care, IV antibiotics and fluids, anticoagulant injections and oxygen support until my lungs recovered. The reason I got so ill with ‘flu, doctors told me, is primarily because I have an autoimmune condition – lupus. I also have asthma, which is also considered a co-morbid condition.
I am certainly ‘at high risk’ from the coronavirus.
The NHS is overstretched. It has already been said that in the event of an epidemic, the NHS would need to “prioritise access to some services in an ethically appropriate way”. That basically means that NHS staff will have to make difficult choices as to who has access to treatment and who is left to die.

Getty Images.
At the moment, people are being told to avoid turning up at hospitals and GP surgeries, in efforts to contain the virus. Nonetheless, a man who recently returned from Italy feeling unwell with a fever waited four days for a call back from NHS 111 clinicians. Dean Hall works on IT projects involving the British Army and he told the BBC he is concerned should he have the coronavirus he might have spread it to military personnel about to deploy.
Others said the advice line gave them confusing, conflicting guidance.
The NHS said that despite high demand, all calls were being answered and the service was hiring extra call handlers. If the demand is high at this stage, imagine how strained things will become if the rates of infection rise and begin to affect whole communities.
“Anyone with concerns about coronavirus should call NHS 111 and – while the service is understandably busy and people may have to wait longer than usual – all calls are being responded to thanks to hard-working NHS staff,” a spokeswoman said.
BBC health editor Hugh Pym said that some calls are coming from people who have visited places outside the list of countries at risk from the virus, adding to the pressures.
However, we don’t know how many people within the UK have been infected. In the countries currently badly affected, the virus had spread quite widely under the radar for weeks before health authorities were alerted to individual cases who needed medical support.
Carole Timms, a nurse from Shropshire who works in care homes, told the BBC that she and a friend were given contradictory advice when they returned from Venice on 20 February. Although they had no symptoms, Timms told NHS 111 she was concerned about the risk to her patients and was told to self-isolate.
But her friend, who works in a college with adults with disabilities, was told it was not necessary. That advice was changed when Timms pointed out the discrepancy.
“If she had just phoned on her own, she would happily have gone back to work when possibly she shouldn’t. Or maybe I’d have got that other advice,” Timms said.
Iwona Dunsford from Milton Keynes said she contacted NHS 111 for testing after she returned from Dusseldorf feeling unwell with a cough and cold – although the city is not considered on the list of high-risk areas for the virus.
She was advised to go to Milton Keynes hospital, but the hospital referred her back to the 111 advice service. Then she was sent to a chemist instead, but the chemist referred her to the hospital.
“I’m OK, but what about the people who are in a worse condition than me? On the TV we’re told that the UK is well prepared for this,” Dunford said.
Clearly we are not all singing from the same hymn sheet.
In Scotland, Alan Kelly said public health authorities initially told him to get tested after he developed flu symptoms following a trip to Milan on 14 February.
But they changed their mind when the government advice for travellers to Italy was updated, because it said only those coming back after 19 February were a concern.
“Surely the prudent thing to do would be to test people with symptoms who have been in the high risk area?” he said.
Yet the government claims that the UK is prepared for all eventualities and is working on containing any outbreaks. That involves spotting cases quickly, isolating them and identifying contacts people have had to stop any spread. This is being done by Public Health England’s (PHE) nine regional teams. Scotland, Wales and Northern Ireland have their own arrangements.
Clearly this isn’t being well co-ordinated on the front line.
It gets worse
The NHS is not prepared for a serious epidemic of COVID-19 in the UK.
Ministers have recently revealed in a parliamentary answers session that there are just 15 available beds for adult extracorporeal membrane oxygenation (ECMO) treatment at five centres across England. The government said this could be increased in an emergency. There were 30 such beds in total available during the 2018-19 winter flu season. That’s not anywhere near enough to cope with a pandemic.
It was also revealed that since the beginning of February there have been just eight “high-consequence infectious disease” beds and around 500 “infectious disease” beds.
For most of last week, there were roughly 3,700 adult critical care beds in England, of which about 80% were occupied. This left 670 such beds free at the peak of occupancy.
However, a NHS England document prepared in November 2017 reveals the system will struggle to cope if more than 28 patients need the treatment, describing that situation as black/critical. That isn’t anywhere near the 20% of the population who may need medical care.
It suggests that if no beds are available “within the designated and surge capacity” in the UK, they might have to be sourced from other countries. However, other countries will also be under strain and are unlikely to have ‘spare’ machines.
The government have also discussed bringing retired medical staff back into service to deal with the virus.
So we have to question the readiness of the NHS to deal with a sharp escalation of coronavirus cases following years of cutbacks and increasing health care rationing.
Answering a Labour MP’s question on Thursday about coronavirus preparedness, Jo Churchill, a health minister, said: “Since April 2013, NHS England has commissioned a total of 15 adult respiratory extra corporeal membrane oxygenation beds from five providers in England, with further provision in Scotland. In periods of high demand, capacity can be increased.”
ECMO treatment is used in the most severe cases of respiratory failure when other treatments are not working. It uses an artificial lung located outside the body to put oxygen into a patient’s blood and continuously pump this blood into and around their body. It has been used to treat COVID-19 cases in China, which is ordering more machines from Germany, according to state media.
The document suggests that if no beds are available “within the designated and surge capacity” in the UK, they might have to be sourced from other countries, for example, from the Karolinska Institute in Sweden. But as I stated, many other countries are either dealing with or preparing for the epidemic. It’s unlikely that there will be a surplus of medical equipment anywhere.
While making no assessment of numbers, Professor Chris Whitty, who is Chief Medical Officer for England, Chief Medical Adviser to the UK Government, Chief Scientific Adviser at the Department of Health and Social Care and head of the National Institute for Health Research, said that if there was a global pandemic it would be impossible for the UK to escape. If that happened, it could mean that the NHS would have to “prioritise access to some services in an ethically appropriate way”, according to the government’s 2011 plan. This could involve postponing non-emergency operations and ultimately, if the outbreak was unremitting, “treating only emergency patients.”
He also said: “Delay is the next stage of what we need to do because if we are going to get an outbreak in the UK – this is an if, not a when – but if we do, putting it back in time into the summer period, away from winter pressures on the NHS, buying us a bit more time to understand the virus better, possibly having some seasonal advantage, is a big advantage.”
When asked how many people in the UK could die, Prof Whitty refused to answer, saying it was difficult to put a true figure on the death rate in China, which “could be less than the 1 per cent reported”. However, it is highly unlikely that China would overstate the mortality rate from the virus.
Over recent years it has become very clear that privately financed health systems fail far too many citizens. Market failures lead to exploitation of ‘healthcare consumers’, an under-investment in public health services and where poorer members of society are systematically excluded from the health care system.
I’ve had severe pneumonia and sepsis once, and that makes it rather more likely I will have both again, though of course, it’s not inevitably because of this particular coronavirus. However, one of the biggest causes of death in people with lupus is pneumonia and sepsis.
The government and NHS simply do not have the facilities to contain many more than a few hundred people. In the event of mass transmissions, responses, according to the government, will be co-ordinated by the government’s Cobra committee and 43 local “resilience forums” in England and Wales. These include Public Health England officials, the NHS, local councils and the emergency services.
Resilience? The power of positive thinking isn’t going to prevent the virus spreading, or some people getting seriously ill.
What we need is an honest government, access to speedy, responsive healthcare, sufficient hospital beds, sufficient numbers of medical staff, ventilators, oxygen cylinders and medications.
I think I will be staying home voluntarily for a while, as much as I possibly can. I will also be investing in some basic medical provisions to try and address any serious symptoms myself, to buy a little time in the event of getting the infection, because I think it’s highly likely that I will have to wait quite a while for access to medical support, should I really need it.
And probably, so will many others, if the worst happens.
—
Further information
Symptoms:
The infection seems to typically start with a fever, followed by a dry cough.
After a week, it leads to shortness of breath and some patients will require hospital treatment. Some people who have chronic medical conditions may develop pneumonia and some may also develop an abnormally aggressive immune response to the virus (sepsis), which is a medical emergency. Septic shock – caused by plummeting blood pressure – can rapidly lead to multiple organ failure and death.
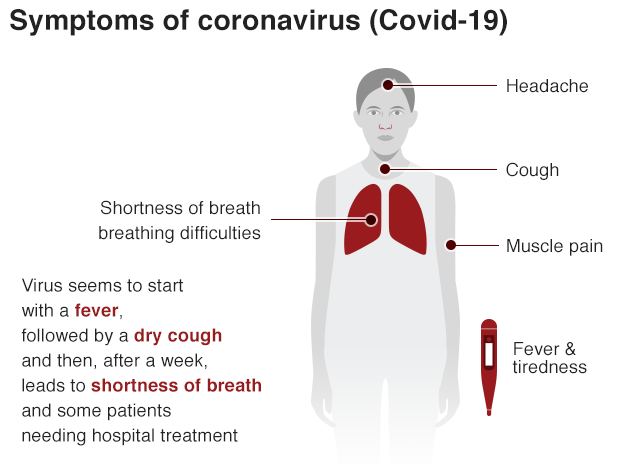
Source: The World Health Organisation (WHO)
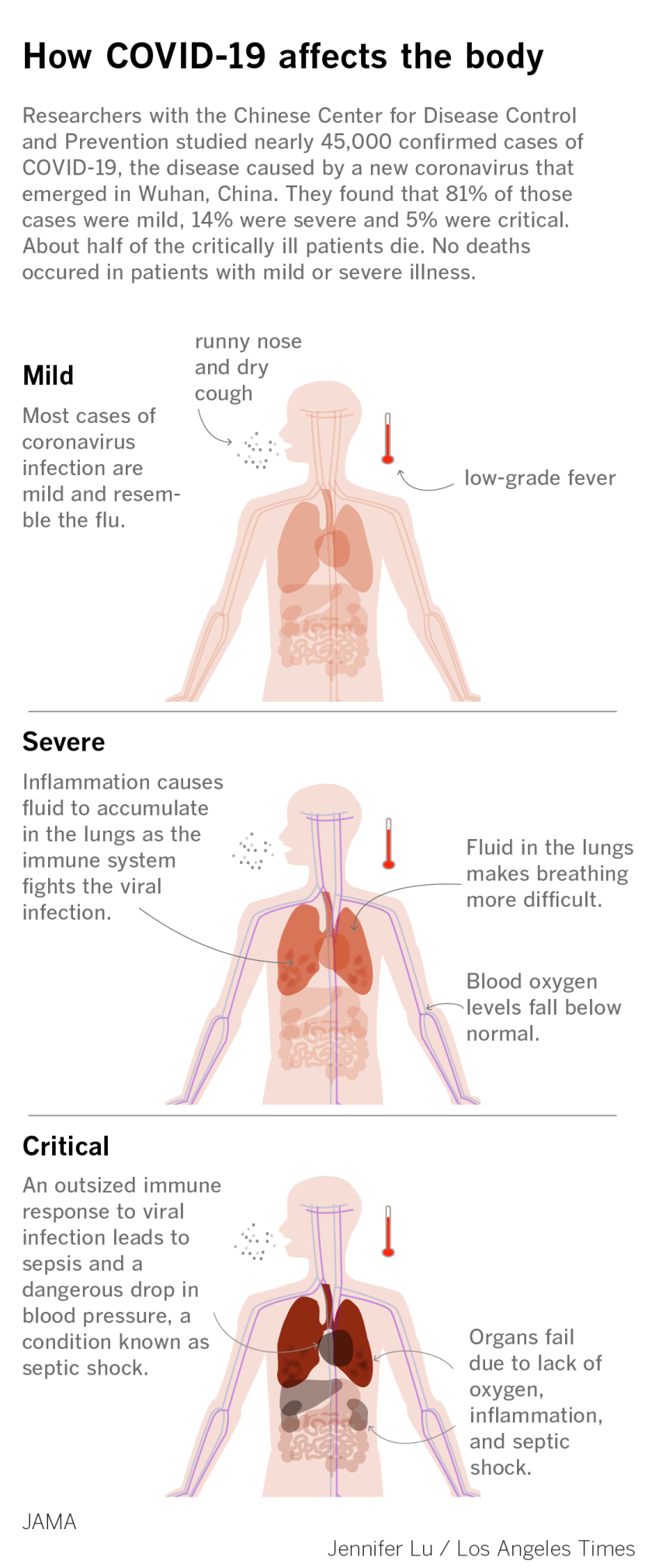
Reducing risk
Because it’s a new illness, health specialists do not yet know exactly how coronavirus spreads from person to person. However, similar viruses are spread in cough and sneeze droplets and aerosols , shaking hands, touching a person who is infected or by touching a hard surface that is contaminated with the virus. Corona viruses generally can survive on surfaces for up to nine days, depending on temperature and humidity.
At temperatures of around 4°C or 39.2oF, certain versions of the coronavirus could remain viable for up to 28 days. At temperatures of 30–40°C (86–104°F), coronaviruses tended to persist for a shorter time. They also tend to survive significantly longer in an environment with 50% humidity than 30% humidity, according to some studies. However, others have contradicted these findings and demonstrated that the viruses thrive best in low humidity.
Disinfect kitchen work surfaces, door handles and other areas that are touched a lot by family members, including taps and the toilet.
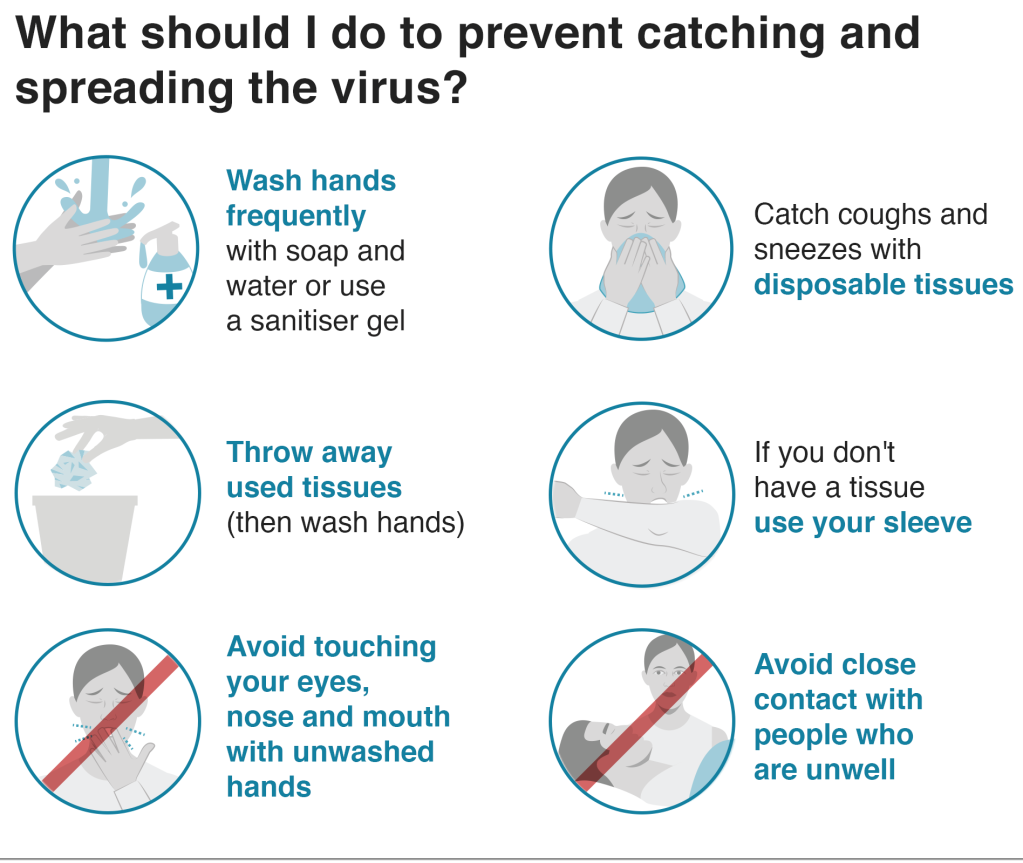
Source: NHS
More people, like you, are reading and supporting independent, investigative and in particular, public interest journalism, than ever before.
I don’t make any money from my research and writing, and want to ensure my work remains accessible to all.
I have engaged with the most critical issues of our time – from the often devastating impact of almost a decade of Conservative policies and growing, widespread inequality to the influence of big tech on our lives. At a time when factual information is a necessity, I believe that each of us, around the world, deserves access to accurate reporting with integrity and the norms of democracy at its heart.
My work is absolutely free from commercial and political interference and not influenced one iota by billionaire media barons. I have worked hard to give a voice to those less heard, I have explored where others turn away, and always rigorously challenge those in power, holding them to account.
I hope you will consider supporting me today, or whenever you can. As independent writers, we will all need your support to keep delivering quality research and journalism that’s open and independent.
Every reader’s contribution, however big or small, is so valuable and helps keep me going. Thanks.


